Smart patch used as blood sugar regulator instead of injections!
Contents

Diabetes :
Diabetes is a disease where blood sugar levels are too high because the body can no longer make or use insulin properly. The condition could lead to serious complications and even death. An estimated 29.1 million Americans have diabetes according to the Centers for Disease Control and Prevention.
There are several types of diabetes which include Type 1, Type 2 and gestational — a type that occurs in pregnant women. All forms of diabetes involve high blood sugar levels.
It’s important to keep blood sugar levels controlled because it can cause serious health problems. It includes kidney diseases, heart problems, skin problems and limb amputations.
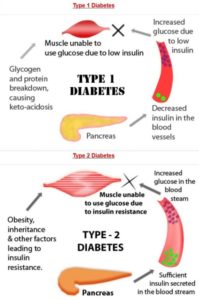
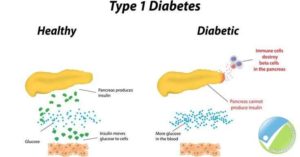
What is Type 1 Diabetes?
Type 1 diabetes occurs when the immune system mistakenly attacks and destroys healthy tissue. An illness, such as an infection or virus like mumps, measles, rubella or the flu, or another trigger can cause the body to turn on itself, mistakenly attacking cells in the pancreas that make insulin.
Type 1 is a life-long disease with no cure and no chance of remission. Treatment involves daily insulin injections. The exact cause of Type 1 diabetes is unknown.
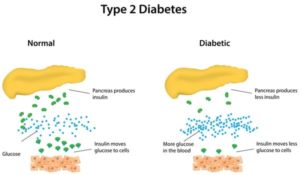
What is Type 2 Diabetes?
Type 2 diabetes is a disease in which your body loses its ability to produce and use insulin, a hormone made by the pancreas that the body uses to convert glucose into energy. Without the right amount of insulin, excess sugar builds up in the body and causes a number of health problems.
Type 2 diabetes is a progressive disease. This means that it may worsen over time and require higher doses of medication or multiple medications to control blood sugar. The pancreas may stop producing insulin altogether, and this means a person with Type 2 will need to inject insulin along with other medications.
What is Gestational Diabetes?
Gestational diabetes is diabetes that happens for the first time during pregnancy. It usually occurs around the 24th week. Gestational diabetes is not the same condition as a person already diagnosed with Type 1 or Type 2 diabetes who then gets pregnant.
A diagnosis of gestational diabetes does not mean that a woman had diabetes prior to conceiving. Moreover, gestational diabetes generally goes away after pregnancy. However, it can increase a woman’s chances of developing Type 2 diabetes later in life. The infant may also be at an increased risk for obesity and Type 2 diabetes.
Pregnant women are typically tested for diabetes during the second trimester of the pregnancy as a part of routine prenatal care. Gestational diabetes is caused by hormones from the placenta that block the body’s normal use of insulin. This prevents the body from regulating the increased blood sugar levels that are usually associated with pregnancy.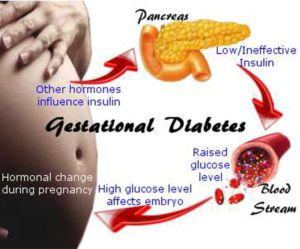
Smart Insulin Patch :
Diabetes affects more than 387 million people worldwide. Patients with type-1 and advanced type-2 diabetes must regularly monitor their blood sugar levels and inject themselves with varying amounts of insulin. This process is immensely painful and imprecise. Injecting the wrong amount of medication can lead to significant complications like blindness and limb amputations Sometimes, it can be even more disastrous such as diabetic comas and death.
Insulin is a hormone that plays a vital role in regulating blood glucose levels. People with type 1 diabetes, as well as advanced type 2 diabetes, require regular insulin injections, as their body either doesn’t produce enough insulin or reacts to it in the wrong way.
Researchers have developed a new type of glucose-sensing patch, which is worn on the skin and delivers insulin in response to sensing high levels of glucose.

Smart insulin patch is one recent project, started in early 2015 that would benefit people with Type 1 as well as those with advanced Type 2 who require insulin. ADA Pathway to Stop Diabetes scientist Zhen Gu, a professor in the Joint University of North Carolina State University Department of Biomedical Engineering, published a paper in the biomedical journal. This paper was termed as the Proceedings of the National Academy of Sciences which describes the development of the new patch that could replace painful and burdensome injections.
The smart insulin patch, made of thin silicon, is about the size of a penny. It includes more than 100 microneedles, each one approximately the size of an eyelash. The microneedles house live beta cells that can sense when blood glucose levels are high and send a rapid release of insulin into the patient’s bloodstream. The live beta cells (cells responsible for making insulin) are said to reduce the risk of complications and last longer than the synthetic insulin that was previously preloaded in the patch.
The final prototype is expected to include glucagon (the hormone responsible for counteracting insulin) into the device as well. This will make the smart insulin patch effective in correcting both high blood glucose levels as well as low blood glucose levels (hypoglycemia), a dangerous potential side effect of taking insulin.
Scientists have tested the smart insulin patch technology in mouse models, where it was discovered that the device was able to effectively lower blood glucose levels for up to nine hours. The positive result paves the way for continuing research in live animals and eventually clinical trials for humans.
How the patch works : 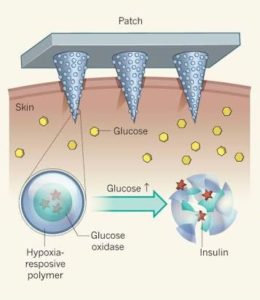
The FreeStyle Libre system works by a 35mm-wide patch which is placed on the back of the upper arm.
A tiny filament – the width of three human hairs – goes through the upper level of the skin and reads the glucose levels in the substance between skin cells, called the interstitial fluid.
The information is transferred from the patch to a digital reader via NFC waves – the same technology used for Oyster cards and contactless card payments.
Where did the story come from?
The study was carried out by researchers from the University of North Carolina and North Carolina State University. It was funded by the American Diabetes Association, and the North Carolina Translational and Clinical Sciences Institute, which is supported by the National Institutes of Health.
The study was published in the peer-reviewed scientific journal Proceedings of the National Academy of Sciences (PNAS).
The UK media’s reporting of the study was patchy. The Mirror fails to mention that the study involved mice, rather than humans. This fact was acknowledged by The Daily Telegraph, though its headline “End in sight for diabetes injections as scientists develop smart patch” is premature, considering the early stage of the research.
How did the researchers interpret the results?
The researchers concluded that this was the first demonstration of a man-made glucose-responsive device using low levels of oxygen as a trigger for regulating insulin release. They say that if this technology is developed for human use, its fast responsiveness could help to avoid blood glucose levels getting too high (hyperglycaemia) or too low (hypoglycaemia).
The challenges in developing an insulin patch :
Insulin patches may seem an obvious form of delivery, however, the challenge in successfully developing an insulin patch has been that insulin is a large molecule and therefore is not usually absorbed by the skin.
Insulin patches therefore require agents to help the insulin pass through the skin and to do so in a controlled and consistent way so as to prevent too high or too low blood glucose levels from occurring.
Conclusion :
The study showed that the patch was capable of reducing blood glucose levels in mice with chemically induced diabetes. This research is at an early stage and as yet, we don’t know how well it works in humans. They will also need to see how long such patches could regulate blood glucose levels for. Although people might prefer patches to injections, they might not want to change them frequently. Researchers will need to look at the long-term effects of wearing these patches in animals, to make sure they are safe and effective enough before testing them on humans.
There is a lot of work going on in the field of diabetes research, looking at developing alternatives to insulin injections. This study has developed another possible approach, and research will likely continue on these patches and other alternatives.
-Shreesha Balan



6 Comments
Pancreas · October 22, 2019 at 3:12 pm
Very informative article, it helped me a lot
Lorrie Roa · November 18, 2019 at 3:31 am
Great post! Thank you for the insightful article. I like the glucose tablets idea, great way to keep them close and without worry about how delicate an alternative might be. I would love to hear more about the significance of the blood glucose levels.
AADass · January 13, 2020 at 10:33 am
Ver Useful post! In today’s world where diabetes is a major problem, this piece of information will guide diabetic patients in the right direction.
Rifat · January 21, 2020 at 9:32 am
What an Great Post. Very interesting topic of the time and I really thrilled to read this. Keep posting such interesting topics.
Nova Biomedical · March 19, 2020 at 8:03 am
Thanks, for sharing a great post. It is really helpful. It’s very useful for diabetic patients.
Zoe Campos · January 1, 2021 at 2:41 pm
Thanks for reminding me that I need to keep my blood sugar levels controlled if I can confirm that I have diabetes. Both my parents have this and I won’t be surprised if I’d get the same diagnosis. Still, I think I shouldn’t wait for the earliest symptoms and I might need to have my blood tested in a nearby lab.